From Consumer Curiosity to Clinical Milestone
Augmented reality healthcare crossed a new threshold when a surgeon completed the first knee replacement using an AR headset in live clinical practice on May 6, 2026. The procedure used Pixee Medical’s Knee+ NexSight system and marked the first time AR headsets surgery moved from carefully staged demos to a real operating room case at Trinity Health Oakland. This milestone comes just days after the platform received FDA 510(k) clearance on April 27, 2026, and follows a CE mark and early use in Europe earlier in the year. Together, these approvals signal that AR medical devices are no longer speculative pilots. They are now regulated tools that hospitals must formally evaluate, with implications for surgical precision, workflow design, and training pathways. For healthcare leaders, the question is shifting from “if” to “how fast” to integrate surgical AR technology into everyday orthopedic care.
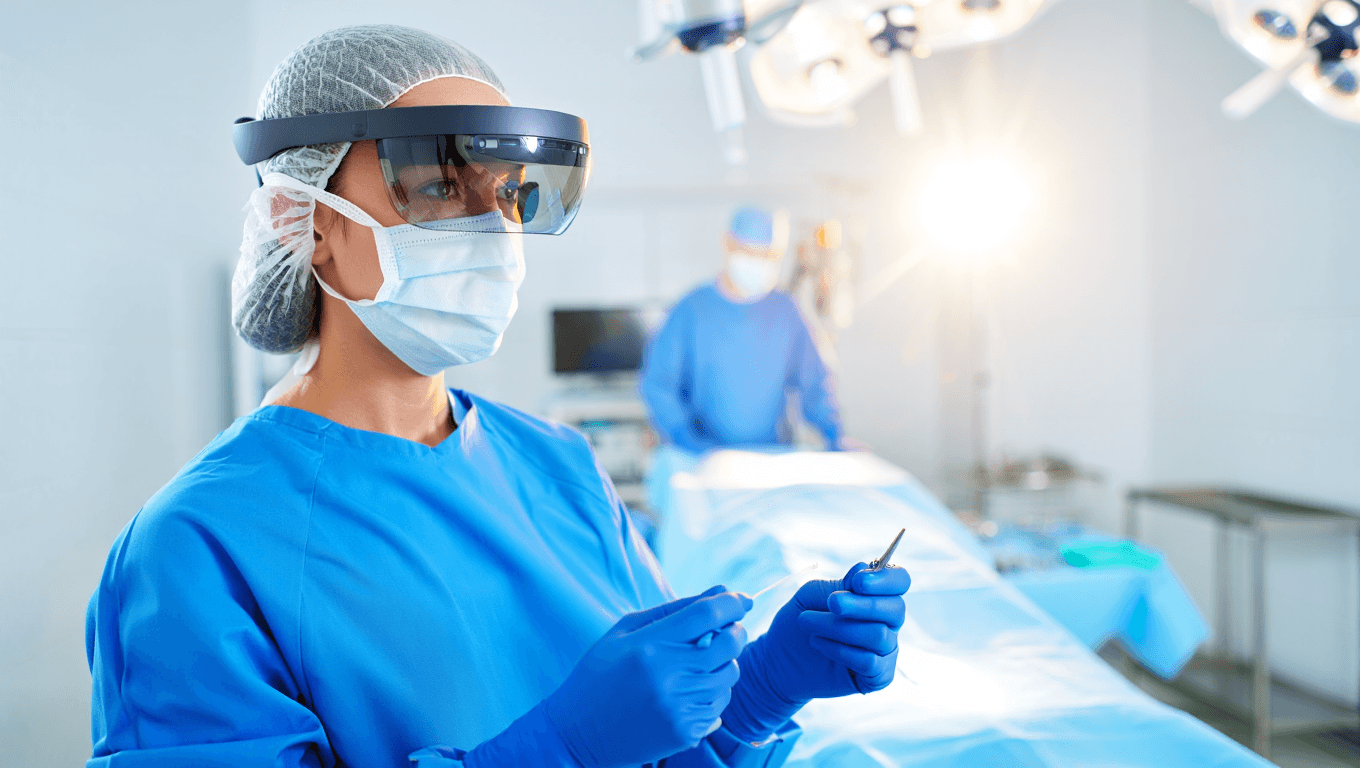
Knee+ NexSight and the New AR-Guided Operating Room
Knee+ NexSight is positioned as a bridge between today’s operating rooms and tomorrow’s fully augmented reality healthcare environment. With its FDA 510(k) clearance, the system can now be used clinically and is marketed as compatible with all primary total knee implants, easing integration with existing supply chains and surgeon preferences. During the inaugural AR headsets surgery case, observers highlighted the value of real-time overlays that support implant positioning and alignment without requiring disruptive changes to core orthopedic workflows. Pixee emphasizes that the platform slots into current routines rather than replacing them, an important point for hospitals worried about OR efficiency and training overhead. Early adopters hope AR guidance will tighten consistency across surgeons and reduce variability in outcomes, while skeptics want peer-reviewed data before large-scale rollout. Either way, the first live case has forced procurement and clinical committees to treat AR medical devices as near-term, not distant, decisions.
A Converging AR Hardware Wave Meets Operating Rooms
The timing of this AR-guided knee replacement is not accidental; it coincides with a broader surge in AR hardware momentum. Across 2026, prototypes, chip deals, and commercial launches are converging, creating a maturing ecosystem that healthcare can plug into. Consumer-focused moves, such as Snap’s Qualcomm-backed glasses roadmap, rumors of Apple smart glasses, and Samsung’s Galaxy XR launch, are pressuring the industry toward lighter, more power-efficient headsets. At the same time, Meta’s pivot toward enterprise and Amazon’s logistics experiments highlight AR’s growing role in professional settings. These trends matter for augmented reality healthcare because they drive faster innovation in optics, comfort, and on-device AI—capabilities that surgical AR technology can repurpose. Hospitals are effectively riding the same hardware wave as consumers and enterprises, but with clinical software like Knee+ NexSight layered on top to deliver procedure-specific visualization and guidance.
Why Healthcare Is Emerging as a Core AR Growth Market
For AR headset manufacturers, healthcare represents a powerful growth vector beyond gaming, messaging, or industrial fieldwork. Operating rooms are ideal environments for AR medical devices: surgeons already rely on imaging, navigation, and complex instrumentation, and they work in controlled, high-value settings where incremental efficiency and precision matter. AR headsets surgery workflows can overlay mechanical axes, bone cuts, and implant alignment directly into the surgeon’s field of view, promising to reduce reliance on bulky navigation towers or repeated manual checks. Orthopedics is a logical beachhead because joint replacement procedures are high-volume and standardized, making benefits easier to quantify. If platforms like Knee+ NexSight demonstrate consistent improvements in implant positioning and reproducibility, they could justify investments in hardware, training, and support. Success in this niche would likely expand AR adoption into other surgical domains, from spine to trauma and beyond.
Barriers Ahead: Training, Evidence, and Reimbursement
The first successful AR-guided knee replacement does not guarantee rapid, universal adoption. Hospitals still face practical hurdles: funding training programs, updating protocols, and ensuring that AR headsets integrate cleanly with sterilization, staffing, and scheduling constraints. Surgeons who watched the May 6 case praised the clarity of AR overlays, but administrators quickly raised concerns about acquisition costs, learning curves, and how payers will treat augmented reality healthcare tools. Early adopters will likely run tightly controlled pilots focused on alignment metrics, operative time, and complication rates, building the evidence needed to justify broader rollout of surgical AR technology. Meanwhile, reimbursement models may lag, forcing institutions to absorb initial expenses while outcome data accumulates. The next phase will be less about headline-grabbing firsts and more about operationalizing AR medical devices—proving that they can consistently deliver better, safer orthopedic surgery at scale.
