From Single-Use Cells to the Body’s Master Builders
Most cells in the body have one job: a skin cell protects, a nerve cell transmits signals, a blood cell carries oxygen. Stem cells are different. They are unspecialized “master” cells with two defining abilities: they can renew themselves through countless divisions, and they can differentiate into many specialized cell types, including muscle, nerve, blood, and skin. This unique combination powers the body’s natural repair system, quietly replacing damaged or aging cells throughout life. In stem cell therapy, scientists and clinicians harness this built‑in repair capacity for targeted tissue repair and cellular healing. Instead of relying only on drugs or surgery to control symptoms, stem cell approaches aim to supply fresh, functional cells exactly where the body needs them most, laying the groundwork for a new era of regenerative medicine.
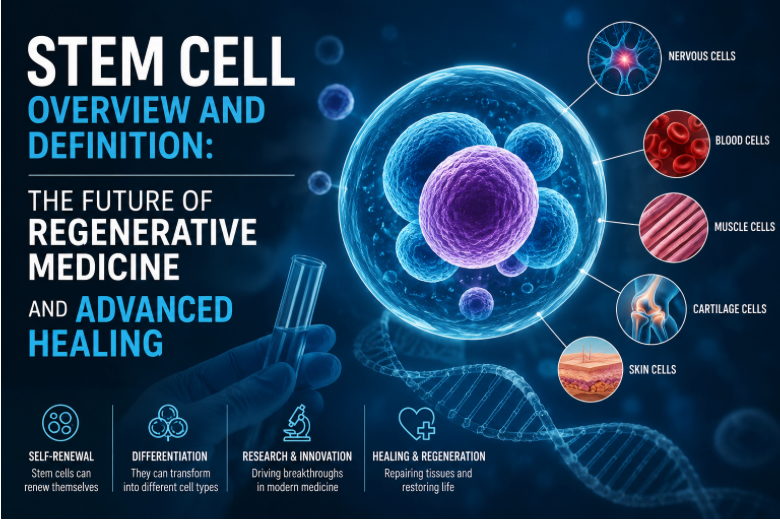
What Makes Regenerative Medicine Different
Traditional treatments often focus on controlling symptoms or slowing disease progression. Regenerative medicine takes a different path: it targets the root problem at the cellular level. By using stem cells and related technologies, the goal is to repair, replace, or regenerate damaged tissues so organs can work more like they did before illness or injury. This shift from symptom management to cellular repair represents one of the most significant transformations in modern healthcare. In conditions where cells are lost, depleted, or malfunctioning, stem cell therapy offers a way to restore function instead of merely compensating for what is missing. Researchers are also combining stem cells with gene editing and tissue engineering, opening possibilities such as lab-grown tissues, personalized treatments, and more precise models for studying complex diseases and testing new medicines.
Beyond Anti-Aging Creams: Real Medical Applications
Stem cells are often marketed alongside cosmetic anti-aging products, but their most profound impact lies far beyond the skincare aisle. In established treatments like bone marrow transplantation for leukemia and lymphoma, healthy stem cells rebuild the blood and immune system after intensive therapies. This same principle of tissue repair and cellular healing is now being explored for serious conditions such as heart disease, Parkinson’s disease, diabetes, spinal cord injuries, and osteoarthritis. Researchers are investigating whether stem cell therapy can restore damaged heart muscle, replace lost dopamine-producing neurons in the brain, or regenerate cartilage in worn joints. While cosmetic uses like skin rejuvenation and hair restoration are being studied, they represent only a small slice of a field focused on restoring critical functions and improving long-term health outcomes.
Types of Stem Cells and How They Are Used
Different medical challenges call for different kinds of stem cells. Embryonic stem cells, taken from very early embryos, can become nearly any cell type, making them powerful tools for research but also a focus of ethical debate. Adult stem cells, found in tissues like bone marrow, fat, and blood, already underpin common therapies for blood disorders and are being tested for joint and cartilage repair. Induced pluripotent stem cells (iPSCs) are adult cells reprogrammed to behave like embryonic stem cells, offering versatility without relying on embryos. Perinatal stem cells, collected from umbilical cord blood and amniotic fluid after birth, are increasingly banked for potential future use. Across these sources, the central aim is the same: enable safer, more targeted tissue repair and expand the possibilities of regenerative medicine.
Promise, Risks, and the Road Ahead
The promise of stem cell therapy is enormous: faster healing after injury, regeneration of damaged tissues, and potentially a future in which lab-grown organs ease donor shortages. Personalized cell-based treatments could match an individual’s biology, improving effectiveness and reducing some complications. Yet the field also carries real risks and unanswered questions. Transplanted cells may trigger immune reactions, fail to integrate properly, or grow in uncontrolled ways, potentially forming tumors. Ethical concerns remain around specific cell sources, and many proposed treatments are still in clinical trials, with long-term safety and benefits under active study. As research advances, stem cells are poised to become a cornerstone of regenerative medicine, shifting our understanding of what it means to heal—from patching problems to rebuilding the body from its most fundamental cellular components.