Where Radiotherapy Fits in a Breast Cancer Treatment Plan
For many people, radiotherapy feels like the moment treatment truly begins, so it can be surprising when it doesn’t start immediately. In a typical breast cancer treatment plan, the sequence is often surgery first, then chemotherapy if needed, followed by breast radiotherapy. Surgery removes the visible tumour; chemotherapy, when indicated, seeks out microscopic cancer cells throughout the body. Radiotherapy after surgery then targets the breast or chest wall and nearby lymph nodes to reduce the risk of local recurrence. Radiation after surgery is usually scheduled once wounds have healed and any chemotherapy cycles are completed. This isn’t because radiotherapy is less important; it’s because tissues need time to recover and because other treatments must be given in a logical order. Understanding this sequence can reduce anxiety when you hear that your breast radiotherapy timing will be weeks, not days, after surgery or diagnosis.
Planning Is Not a Delay: It’s the Treatment Before the Treatment
The first “radiotherapy day” often feels anticlimactic. You arrive expecting beams of radiation and instead have a CT scan, some careful measurements, and then are sent home. Nothing seems to happen. In reality, this is when modern breast radiotherapy is being built around your body. The planning CT is not checking whether the cancer has changed; it is mapping your anatomy in the exact position you will be treated. Arm position, chest wall shape, breast mobility, and even breathing patterns all affect how radiation dose falls on the breast and nearby organs such as the heart and lungs. Precision geometry comes first, because geometry determines dose. After you leave, specialists contour target areas and organs at risk, run dose calculations, and verify the plan. This technical work during the radiotherapy waiting period is deliberate: it reduces error before any exposure begins.
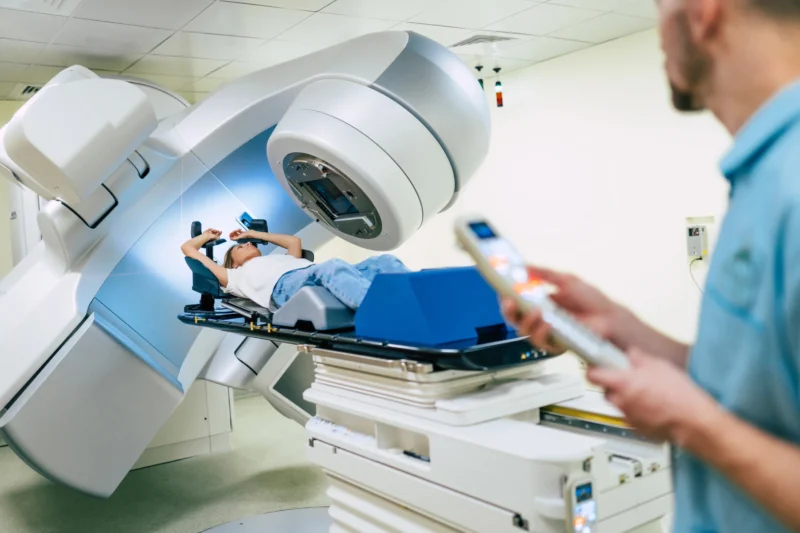
Why the Waiting Period Is Clinically Necessary
To patients, the days or weeks between surgery, planning scans, and the first treatment can feel like alarming silence. Clinically, that time is doing important work. Surgical sites must heal to lower the risk of complications and to ensure the breast or chest wall is in a stable shape for accurate targeting. If chemotherapy is part of your pathway, your team will usually complete it first, so radiotherapy does not interrupt crucial systemic treatment. Meanwhile, your care team is refining the plan: adjusting doses, fine-tuning angles, and checking that vulnerable organs are protected as much as possible. Radiotherapy is one of the most protocol-driven treatments in oncology; nothing is rushed and nothing is improvised. A short, planned radiotherapy waiting period does not automatically mean worse outcomes. In many cases, it reflects a careful balance between safety, precision, and effectiveness for your specific situation.
How Technology Makes Use of Every Day Before Treatment Starts
Behind the scenes, the time between your planning scan and first session is filled with technology-driven work. Advanced imaging merges your planning CT with previous scans to give a detailed 3D view of your breast and surrounding structures. Treatment-planning software then simulates thousands of possible beam arrangements to shape radiation closely around the target while sparing healthy tissue. Modern radiotherapy machines can deliver highly conformal dose patterns and may adapt to your breathing or subtle movements, but they rely on a rock-solid plan created beforehand. Quality assurance checks ensure the machine delivers exactly what was calculated. This means the apparent lull is actually an intensive design and safety phase. Understanding that this invisible technical effort is happening can reframe the waiting period from “nothing is being done” to “my team is customizing my treatment as precisely as possible.”
Using the Waiting Period for Patient Empowerment
Although you cannot fast-forward the start of radiotherapy, you can use the waiting period to feel more prepared and in control. Bring a written list of questions to each visit, such as: What is the goal of my breast radiotherapy? How long after surgery will radiation start in my case? Which side effects should I expect, and how will we manage them? Clarifying your breast cancer treatment plan can turn uncertainty into informed participation. Digital health tools can help too. Calendar and reminder apps reduce the stress of tracking appointments. Symptom-tracking apps let you log fatigue, skin changes, or mood shifts to discuss with your team. Secure patient portals, where available, allow you to review reports and message your clinicians. Used wisely, these tools turn a passive-feeling radiotherapy waiting period into an active phase of learning, organizing, and building the support you need for treatment.
