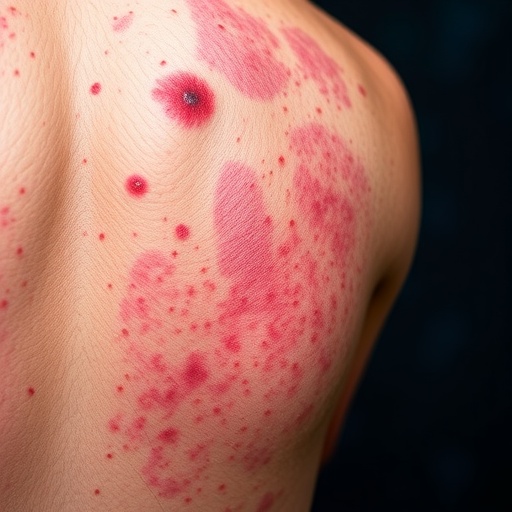
From One-Size-Fits-All to Personalized Psoriasis Treatment
Psoriasis is an autoimmune skin condition affecting around 125 million people worldwide, yet it rarely behaves the same way in any two patients. For decades, dermatologists relied on a trial-and-error approach, cycling through creams, pills and injections to find something that worked. Today, advances in genetic testing for skin conditions and detailed immune analysis are changing that model. Researchers have mapped multiple genetic susceptibility loci, including variants in the major histocompatibility complex such as HLA-C06:02, that influence how the disease starts and progresses. These discoveries underpin a new era of personalized psoriasis treatment, where a person’s unique genetic and immunological profile guides clinical decisions. Instead of grouping all patients under a single label, dermatologists can now recognize distinct molecular subtypes of psoriasis, each with its own triggers, immune pathways and likely treatment responses. This shift marks the beginning of truly individualized care.
Immunogenetics: Understanding the Roots of Psoriasis
Immunogenetics psoriasis research focuses on how specific genes shape the immune responses that drive psoriatic plaques. Key variants help explain why some people develop the disease and why their skin behaves in a chronically inflamed way. HLA-C06:02, one of the strongest genetic risk factors, influences antigen presentation to immune cells and is closely tied to psoriasis susceptibility. Other genes, such as IL12B and TNIP1, highlight critical inflammatory pathways. IL12B encodes a shared subunit of interleukins 12 and 23, cytokines that push T-helper cells toward pro-inflammatory behavior. TNIP1 regulates NF-κB signaling, a central controller of immune activation. Together, these genes feed into the IL-23/IL-17 axis, a core network that promotes abnormal keratinocyte proliferation and immune cell infiltration. By revealing how these pathways interact, immunogenetics clarifies the root causes of disease in individual patients and provides a rational basis for targeted psoriasis therapy.
Genetic Testing Skin Conditions for Tailored Diagnosis
In modern dermatology, genetic testing for skin conditions like psoriasis is moving from research labs into routine practice. High-throughput sequencing and powerful bioinformatics tools can now detect risk variants such as HLA-C06:02 and polymorphisms in IL12B or TNIP1 with increasing speed and accuracy. When combined with immunological assays, this information allows clinicians to classify psoriasis into distinct immunogenetic subtypes rather than relying solely on how lesions look on the skin. Personalized diagnosis based on these signatures helps predict how aggressively a patient’s disease might evolve, which immune pathways are most relevant, and what comorbidities—such as joint or cardiovascular involvement—may need attention. Importantly, this approach supports more precise, evidence-based treatment planning. Instead of applying generic algorithms, dermatologists can align interventions with each patient’s molecular profile, improving the odds of early control, reducing unnecessary exposure to ineffective drugs and enhancing long-term outcomes.
Targeted Psoriasis Therapy and Predicting Treatment Response
Insights from immunogenetics have directly inspired a new generation of targeted psoriasis therapy. Biologic agents that neutralize IL-17, IL-23 and TNF-α are designed to interrupt the very cytokine networks identified as central to disease pathogenesis. For example, blocking IL-23 can dampen downstream IL-17 production, easing chronic skin inflammation and reducing plaque thickness. Because these drugs act on defined molecular pathways, genetic and immunological testing can help predict which patients are most likely to benefit from each option. A person whose immunogenetic profile strongly implicates the IL-23/IL-17 axis might be a particularly good candidate for IL-23 or IL-17 inhibitors, whereas another with a different signature could respond better to TNF-α blockade. This ability to anticipate treatment response helps avoid prolonged trials of ineffective therapies, shortens the time to disease control and supports more efficient, patient-centered care.
What Personalized Psoriasis Treatment Means for Patients
For patients, personalized psoriasis treatment is about far more than genetic jargon or laboratory reports. Understanding that their condition arises from specific genetic predispositions and immune pathways can demystify the disease and reduce self-blame. Genetic and immunological findings also clarify how environmental factors—such as infections, stress or lifestyle choices—interact with underlying susceptibility, giving patients practical levers to reduce flares alongside medication. As biomarkers of disease activity and therapeutic response are refined, monitoring may become more dynamic, allowing clinicians to adjust treatment before visible relapses occur. Ultimately, this precision approach can reduce side effects, limit unnecessary therapies and address associated problems like joint or cardiovascular involvement more proactively. The ongoing integration of immunogenetics into clinical protocols signals a future in which each person’s psoriasis care is tailored to their unique biological profile and evolving needs.