What Stem Cells Are and Why They Matter
Stem cells are the body’s master cells: unspecialized cells capable of both self-renewal and differentiation into many specialized cell types. Unlike ordinary cells that perform a single role, stem cells can become nerve, muscle, blood, or skin cells depending on the signals they receive. This unique combination of self-renewal and flexibility underpins their role as the body’s natural repair system. When tissues are damaged or cells age, stem cells help replenish what is lost, supporting cellular regeneration and long-term tissue health. In medical science, this makes them powerful tools for stem cell therapy, where carefully prepared stem cells are introduced to help restore function or replace diseased cells. Understanding these fundamentals is essential for anyone interested in regenerative medicine, because every emerging treatment—from advanced tissue repair approaches to organ engineering—builds on these core biological capabilities.
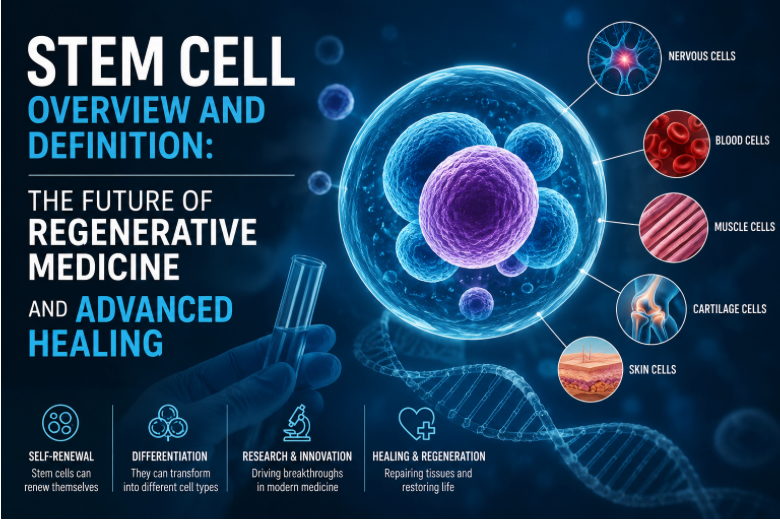
Different Types of Stem Cells and How They Work
Not all stem cells are the same. Embryonic stem cells, taken from very early-stage embryos, can develop into nearly any cell type in the body, making them highly versatile for research. Adult stem cells live in tissues such as bone marrow, fat, and blood, where they help maintain and repair specific organs, and are widely used in transplants for blood disorders. Scientists have also learned to reprogram ordinary adult cells into induced pluripotent stem cells, which behave much like embryonic cells without requiring embryos. A fourth category, perinatal stem cells, comes from umbilical cord blood and amniotic fluid collected after childbirth and can be stored for possible future use. In all these cases, stem cells respond to signals from injured or diseased tissues, migrate to the affected area, and differentiate into the cell types needed for healing and tissue repair.
From Blood Disorders to Tissue Repair: Current Clinical Uses
Stem cell therapy is already part of mainstream care in some areas and rapidly evolving in others. The best-established use is in treating blood disorders such as leukemia and lymphoma. Here, healthy stem cells—often from bone marrow—rebuild the patient’s blood and immune system after intensive treatments like chemotherapy. Beyond blood disease, researchers are testing regenerative medicine strategies for heart disease, Parkinson’s disease, diabetes, spinal cord injuries, and osteoarthritis. The goal is to restore lost function by replacing damaged cells and supporting long-term cellular regeneration. In orthopedics and aesthetic medicine, stem cells are being investigated for joint repair, cartilage regeneration, skin rejuvenation, and hair restoration. These therapies aim to enhance the body’s own healing response rather than simply masking symptoms, representing a shift toward biologically guided repair instead of purely mechanical or pharmaceutical solutions.
Regenerative Medicine, Strategic Partnerships, and Patient Access
Regenerative medicine uses stem cells, bioengineered materials, and biological signals to repair, replace, or enhance damaged tissues and organs. As this field matures, strategic collaborations between hospitals, research groups, and specialized providers are becoming crucial. Partnerships—such as those between clinical innovators like LifespanningRx and RegenTherapy—can combine scientific expertise, advanced laboratory capabilities, and structured patient programs. This makes it easier to translate complex science into accessible treatment pathways, including evaluation, enrollment in regenerative programs, and long-term follow-up. Healthcare institutions engaged in advanced stem cell research help validate protocols, track outcomes, and refine safety standards. The result is a more integrated ecosystem where patients gain earlier access to evidence-based regenerative options, while clinicians receive better tools and data for tailoring therapies. Together, these alliances are accelerating the delivery of sophisticated tissue repair and cellular regeneration strategies to real-world patients.
Promise, Risks, and the Paradigm Shift in Chronic Care
Stem cell therapies offer the possibility of treating chronic conditions and age-related decline at their biological roots rather than only managing symptoms. By actively promoting tissue repair and cellular regeneration, they hint at a paradigm shift: medicine that restores function through living cells. Potential benefits include more personalized treatments, fewer organ shortages if lab-grown tissues become viable, and better tools for studying complex diseases in the lab. Yet, important challenges remain. Some sources of stem cells raise ethical questions, and the immune system can reject transplanted cells. If cell growth is not tightly controlled, abnormal tissue or tumors could develop. Many applications are still in clinical trials, and long-term safety data are being carefully collected. For health-conscious readers, the key is cautious optimism—embracing the promise of regenerative medicine while insisting on scientifically validated, responsibly delivered stem cell therapy programs.